All about inflammation March 2020 radio talk with Zulaikha and Sue
We need to appreciate that inflammation is a protective mechanism. Pain is a warning, so rather attend to the source of the pain if it persists instead of continuously taking pills to switch it off. Acute inflammation is short-lived and usually no treatment is necessary. But our thoughts and emotions also affect the immune system and hence a state of inflammation. Even a suggestion about a pandemic virus can set off the inflammatory response that favours the onset of a respiratory crisis.
Q: We talk about inflammation and take medications to reduce it. So tell us – what exactly is inflammation?
Primary or temporary inflammation is a defensive mechanism that is triggered by the immune system to help us cope with whatever it is that is perceived as a threat to us. The immune system releases pro-inflammatory cytokines – chemicals that help us to deal with a pathogen such as a virus, bacteria or other microbe. Other triggers for cytokines include bites, stings, splinters, bumps, poisons, cuts and other injuries.
We experience the following:
Pain: The inflamed area is likely to be painful, especially to the touch. Chemicals that stimulate nerve endings are released, making the area more sensitive.
Redness: This occurs because the capillaries in the area are filled with more blood than usual.
Immobility: There may be some loss of function in the region of the inflammation. The body prevents the use of the injured limb for instance, to prevent more injury.
Swelling: This is caused by a build-up of fluid. Swelling can also help to immobilise an injured finger joint and hold it in place. The throat closed up and swells to prevent further ingestion of a poison.
Heat: More blood flows to the affected area, and this makes it feel warm to the touch, but increased circulation enables more white blood cells to reach the area to kill microbes and other pathogens.
Q: In the first aid kit we have aspirins and other pain killers. Is it a good idea to keep using them for days on end?
This type of acute inflammation is temporary – a response to fix the problem area and prevent further damage. For instance, if a bee stings you it produces all these symptoms. The pain is acute but will go away when the venom is dissipated – increased circulation, swelling. An analgesic will ease the pain in the meantime but usually we are advised that if symptoms persist one should not use them continuously and rather see a doctor. In the case of toothache, the pain and swelling may not just go away, due to a tooth infection or a more chronic type of inflammation.
Q: What is chronic inflammation?
This refers to long-term inflammation and can last for several months and even years. It can result from:
• Failure to eliminate whatever was causing an acute inflammation
• An autoimmune disorder that attacks normal healthy tissue, mistaking it for a pathogen that causes disease
• Exposure to a low level of a particular microbe or irritant, such as an industrial chemical, over a long period
Examples of diseases and conditions that include chronic inflammation:
• Asthma (irritant in the air)
• Chronic peptic ulcer (caused by low stomach acid)
• Tuberculosis 9a bacterium)
• Rheumatoid arthritis (autoimmune)
• Periodontitis ( poor oral hygiene)
• Ulcerative colitis and Crohn’s disease
• Sinusitis (airborne allergen)
• Active hepatitis (liver pathogen – flukes)
Q: Why is inflammation to blame for most of our chronic diseases?
Cytokines, our pro-inflammatory chemicals are also released by stress – an imagined enemy. So, according to doctors, if you’re stressed you’ll release more of these chemicals, increasing the amount of inflammation in your body, leading to medical issues such as heart attack, stroke, or even cancer. Cytokines are also released in response to physical or psychological stress and can trigger depression, and worsen the episodes. Exposure to stress triggers immune cells in the brain, leading to the rewiring of neural circuits and setting off of mood symptoms. Inflammatory Bowel Disease (IBD) IBD is an umbrella term for inflammation-linked conditions that affect the gastrointestinal system, including Crohn’s disease and ulcerative colitis. Both are exacerbated by stress, which affects the body’s normal secretion of digestive enzymes, and can interfere with how you digest food, absorb nutrients, and rid the body of waste.
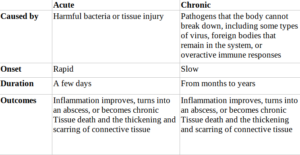
The following table shows the key differences between acute and chronic inflammation:
Q: What type of medications are used to reduce inflammation?
Anti-inflammatory medications
Non-steroidal anti-inflammatory drugs (NSAIDs) can be taken to alleviate the pain caused by inflammation.
They counteract an enzyme that contributes to inflammation. This either prevents or reduces pain.
Examples of NSAIDs include naproxen, ibuprofen, and aspirin, which are available to purchase online.
Avoid the long-term use of NSAIDs unless advised by a doctor. They increase a person’s risk of stomach ulcers, which can result in severe, life-threatening bleeding.
NSAIDs may also worsen asthma symptoms, cause kidney damage, and increase the risk of having a stroke or heart attack.
Acetaminophen, such asparacetamol or Tylenol, can reduce pain without affecting the inflammation. They may be ideal for those wishing to treat just the pain while allowing the healing factor of the inflammation to run its course.
Corticosteroids
Corticosteroids, such as cortisol, are a class of steroid hormones that prevent a number of mechanisms involved in inflammation.
There are two sets of corticosteroids:
Glucocorticoids: These are prescribed for a range of conditions, including:
arthritis
temporal arteritis
dermatitis
inflammatory bowel disease (IBS)
systemic lupus
hepatitis
asthma
allergic reactions
sarcoidosis
Creams and ointments may be prescribed for inflammation of the skin, eyes, lungs, bowels, and nose.
Q: Are there any research-backed ways to reduce stress?
Relaxing activities like yoga, and meditation, going for walks, breathing exercises, playing music, dancing, gardening all reduce cortisol levels and therefore stess related inflammation.
Q: What herbs can we take and is there a diet to help with inflammation?
Ginger, turmeric, devil’s claw are good. Bromelain and pineapples are also effective.
https://naturefresh.co.za/diets-recipes-categories/medicinal/
https://www.medicalnewstoday.com/articles/248423
https://www.everydayhealth.com/wellness/united-states-of-stress/link-between-stress-inflammation/